Mark Greer has had several close calls in his life — he was bucked from a horse once and on another occasion fell 30 feet onto concrete — but he says his heart emergency last fall was the scariest.
The 61-year-old from rural East Texas was airlifted 60 miles from the city of Commerce to Methodist Richardson Medical Center in September after going into cardiogenic shock, a life-threatening condition where the heart isn’t able to pump out enough blood to meet the body’s demands.
“I said my prayers because I thought this was it,” he recalls. “This is an experience I never want to repeat.”
From prevention to advanced procedures, trust your heart to the innovative, personalized care that Methodist provides. Visit MethodistHealthSystem.org
The answer to Mark’s prayers involved getting to a hospital with the expertise and equipment capable of treating his heart condition, says Asad Mohmand, MD, interventional cardiologist on the medical staff at Methodist Richardson.
“This is one of those cardiac emergencies that, if it’s not recognized and treated in a timely fashion, can rapidly spiral into shock and subsequently death,” Dr. Mohmand says.
Mark credits Dr. Mohmand and his team with saving his life.
“I could not have asked for a better team for this type of situation,” he says.

BAD WAY TO GO GRAY
One day last fall, Mark was taking a lunch break at the plumbing supplies company where he works with his wife, Rita. He had been feeling ill that morning, and his boss suggested he talk to his wife because he looked gray.
“As soon as I walked into her office, her eyes popped out and she said, ‘Oh my goodness, what’s wrong with you?'” Mark recounts.
Ultimately, Rita called for help, and an ambulance transported Mark to a nearby hospital. Doctors there recognized the problem on a CT scan but didn’t have the resources or expertise to help him. So Mark was placed on a helicopter, heading straight for Methodist Richardson. Unfortunately, there was no room for his wife on the helicopter.
“She had to drive from our place over in East Texas to Richardson, and she almost beat the helicopter there,” Mark jokes.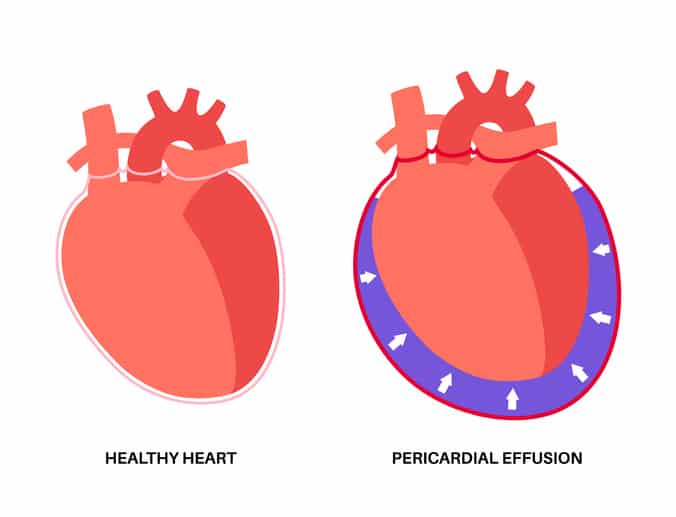
JUMPING INTO ACTION
Paramedics notified the hospital en route, allowing Dr. Mohmand and the specialized staff from the cardiac catheterization laboratory to prepare for his arrival. They even parked an echocardiogram machine in the hallway near the helipad, so that the gravity of Mark’s condition could be assessed as soon as he landed.
“Our cath lab team is always on call for these emergencies,” Dr. Mohmand says. “We work efficiently as a unit as every second is crucial. We had all the necessary equipment ready to go.”
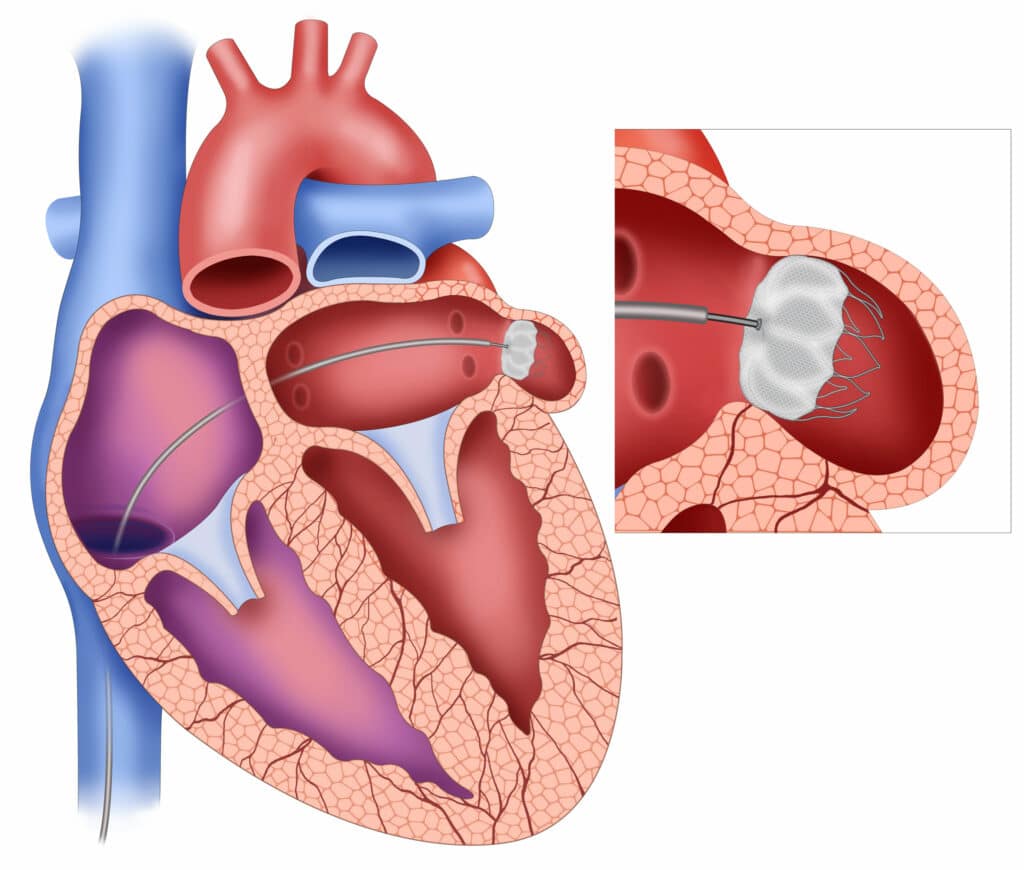
He confirmed that Mark was experiencing something known as pericardial tamponade. The protective sac covering his heart was filled with fluid — mostly blood — compressing it and preventing it from filling or pumping properly.
Mark’s condition was possibly exacerbated by the blood-thinning medications he was prescribed weeks earlier to help with blood clots in his legs.
In the cath lab, Dr. Mohmand inserted a needle through Mark’s chest wall into the pericardial sac to quickly remove the fluid around his heart. Mark says he began feeling better within minutes, and his blood pressure, which had dropped to 70 millimeters of mercury (mm Hg), returned to 140 mm Hg.
“I could just feel the pressure getting off me,” he says, “and I could finally breathe again.”

ON THE MEND
Mark stayed in the hospital for a few nights of careful monitoring before he was deemed well enough to go home. Rita stayed by his side the entire time.
“She was pretty pleased at the hospital with all the different people checking on me,” Mark says. “I can’t even think about having better nurses.”
The couple were relieved when Dr. Mohmand cleared his health in a follow-up appointment a week later. Now, Mark is back home and on the job again, often working from dawn to dusk — and sometimes beyond. He says he hopes his emergency will serve as a cautionary tale for others in his situation.
“I hope my story makes an impression on them and helps them realize they need to take their health seriously,” he says.