Breast cancer is the most common cancer among American women, and younger people are increasingly at risk, with diagnoses among women in their 40s rising 2% each year between 2015 and 2019.
That’s why this spring, an influential task force recommended women start getting mammograms at age 40, rather than 50. But that’s only for women at average risk. Patients with more risk factors should take extra precautions, says Katrina Birdwell, MD, FACS, breast surgeon on the medical staff at Methodist Dallas.
“If a woman knows she’s at high risk for breast cancer, she should not wait until 40 to get a mammogram,” she says. “She should get high-risk screening before that. This could include breast ultrasounds, breast MRIs, and mammograms, typically starting at age 30.”
Ideally, a woman in her mid- to late 20s should get a risk assessment telling her when it’s time to start getting a breast exam, Dr. Birdwell says. An early warning system is especially crucial with breast cancer, which has a five-year survival rate of 99% when it’s detected before it spreads. That drops to 30% once the cancer spreads to the lymph nodes.
“Mammograms provide patients a better hope for survival, as well as several treatment options if the cancer is found early,” Dr. Birdwell says. “If we’re not screening women between 40 and 50, we are missing opportunities.”
The key to preventing breast cancer is managing your risk factors. Take our health risk assessment. Visit MethodistHealthSystem.org
RACIAL DISPARITIES
That’s true for all women, but it’s especially relevant for African-Americans younger than 50, whose mortality rate from breast cancer is twice as high as it is for white women.
“Young African-American women disproportionately get triple negative, the most aggressive kind of breast cancer,” Dr. Birdwell says. “It’s a type that grows and spreads quickly, is hard to treat, and doesn’t have the three receptors usually found in breast cancers that doctors target for treatment.”
It’s unclear why the death rate among African-American women is 40% higher than white women, even though the incidence of breast cancer among white women is slightly higher: 133 cases per 100,000 white women compared with 127 per 100,000 black women.
“We don’t have a clear-cut answer to why that is,” Dr. Birdwell says. “What we do know is that there were women in that 40-50 age group who were developing cancers that we could have detected before they became a higher stage.”
Here’s what else you need to know about the risks and the changing recommendations:

RISK FACTORS
About one in eight American women will be diagnosed with breast cancer in their lifetimes. What’s more, the disease claims the lives of about 42,000 women each year, making it the second-leading cause of cancer death among women.
Having a family history of the disease can raise the risk for both women and men, but your risk is determined by several factors, including age, reproductive history, being overweight or obese, and the presence of certain genetic mutations.
Women who aren’t physically active or become overweight or obese after menopause tend to have a higher risk. So, too, do patients who take certain oral contraceptives and those who undergo hormone replacement therapy during menopause.
Of course, having a risk or two doesn’t mean you will get the disease. After all, most women won’t get breast cancer, regardless of their risk factors, even if a mammogram turns up a lump.
“If your breast screenings come back positive, try not to panic,” Dr. Birdwell says. “Most breast lumps aren’t cancer. But just to be safe, if you notice any concerning changes or lumps in your breasts, schedule a checkup with your healthcare provider.”

FALSE POSITIVES
False positives are one of the key reasons why experts have diverged on when women should start getting mammograms.
“It’s not uncommon for mammograms, ultrasounds, and MRIs to pick up things that look like cancer, but really aren’t,” Dr. Birdwell says.
The U.S. Preventive Services Task Force, the same group that lowered its recommendation for routine mammograms to start at 40, took a different stance in 2009 when it recommended against women ages 40-49 from getting a routine breast exam and reduced how frequently it recommended women age 50 and up get examined.
Among the reasons cited was the proliferation of false positives, which can be costly, cause mental distress, and expose women to risks of unnecessary medical procedures. But now experts appear to agree that the benefits of early detection outweigh the costs of unnecessary tests and potential false positives.
What’s more, technological advancements like digital breast tomosynthesis, also known as “3D mammography,” can make exams more precise, especially for women with denser breasts, who tend to have a higher risk for false positives.
“When it comes to dense breasts, 3D mammograms help us a ton with clarifying the X-ray,” Dr. Birdwell says. “It provides layers of pictures that help us see through dense breasts.”
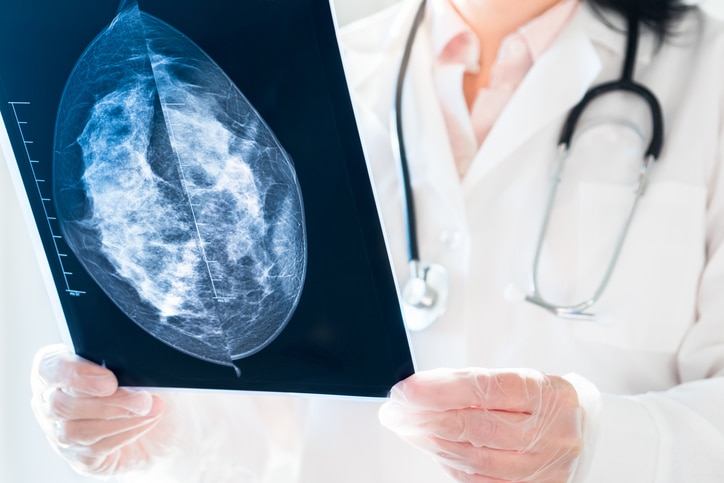
3D MAMMOGRAMS
While a traditional 2D mammogram takes pictures of each breast from two angles, tomosynthesis takes pictures from many different views while moving over the breast. Computer software then combines the scans to form a 3D image.
The high-level detailing makes it easier for a radiologist to see through overlapping breast tissue and determine whether further testing is necessary.
And while mammograms, whether 2D or 3D, remain the gold standard to detect early signs of breast cancer, self-examinations are also important. About 40% of diagnosed breast cancers are detected by women who felt their lump, according to the National Breast Cancer Foundation.
“Familiarizing yourself with your breasts can help you know what your normal is and what’s abnormal,” Dr. Birdwell says. “It’s good for women to examine themselves once every month.”






