More than 35 million Americans live with chronic kidney disease, whether they know it or not, and those numbers seem likely to keep rising, along with diabetes and high blood pressure — the two biggest causes of the disease.
The kidneys are the human body’s filtration system, flushing waste, toxins, and extra fluid out of the blood through the urine. When the tiny filters, or nephrons, inside these organs malfunction, there are often no symptoms until it’s too late.
“Acute kidney failure happens suddenly, whether because of dehydration, infection, or kidney stones, and it’s 100% reversible,” says Srividya Venkataraman, MD, nephrologist on the medical staff at Methodist Charlton Medical Center. “Chronic kidney disease, on the other hand, is a silent killer because people are often unaware they have it until they’ve lost 75% to 80% of their kidney function.”
Dr. Venkataraman sat down with a group from Methodist Generations to discuss the warning signs of chronic kidney disease and tell patients how to avoid causing permanent damage to their kidneys.
COMMON SYMPTOMS
We have two kidneys for a reason: If one is damaged or otherwise compromised, the other picks up the slack. That’s why it’s possible to donate a kidney and still live a normal life.
But that extra capacity also means it’s less noticeable when things go wrong with one kidney because its twin compensates for the lost function.
“When you have heart problems, you have chest pains, and when you have stomach problems, you have nausea,” Dr. Venkataraman says. “Kidney problems often go unnoticed because there are two kidneys. They try to compensate until the function drops below 15%.”
By then, patients may require a transplant or dialysis, a procedure where a machine is used to remove waste and excess fluid from the blood because a patient’s kidneys are overwhelmed. That’s when they may experience one or more of the following symptoms:
- High blood pressure and fatigue
- Itchy skin and difficulty urinating
- Metallic taste in the mouth
- Nausea, vomiting, and loss of appetite
- Swelling and shortness of breath caused by fluid retention
Detecting the disease at earlier stages, when treatment can still preserve healthy kidney function, is crucial for avoiding kidney failure and dialysis.
HOW IT’S DETECTED
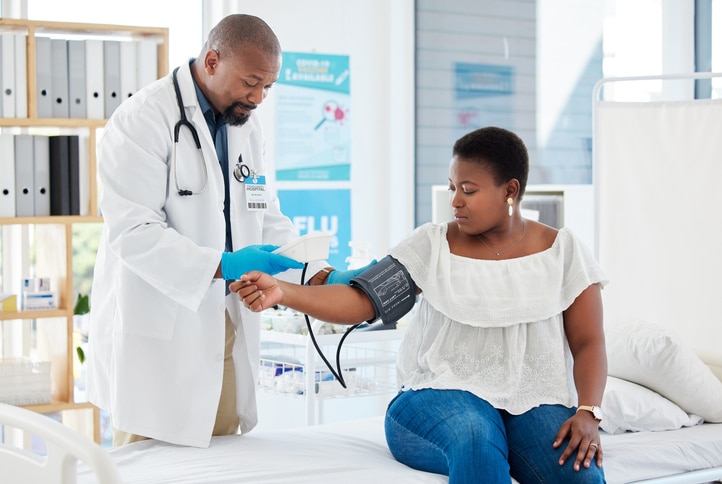
Now for the good news: Chronic kidney disease can be detected through simple blood and urine tests, no invasive procedures, poking, or prodding necessary.
“This can be done at your primary care doctor’s office,” Dr. Venkataraman says. “You don’t even need to fast before giving your blood sample.”
The first thing a doctor will look for is blood or other proteins in the urine. That would suggest a problem with the kidneys’ ability to filter those substances.
“Think about it like a coffee filter: If there are coffee grounds in your cup, there’s something wrong with the filter,” Dr. Venkataraman says. “Normally, there is no protein, no blood in the urine.”
Another sign the kidneys aren’t doing their job is elevated creatinine levels in the bloodstream. Not to be confused with the amino acid creatine, this waste product is created by the breakdown of muscle tissue in the body and normally gets flushed out in the urine.
“Your doctor will use the result of your creatinine test, combined with your age, gender, and other factors, to calculate what’s called an estimated Glomerular Filtration Rate, or eGFR,” Dr. Venkatamaran says.
An eGFR between 60 and 120 is considered normal, while 15 to 60 may signify kidney disease. An eGFR under 15 is a sign of kidney failure. Knowing your kidney numbers is just as critical as understanding your cholesterol levels and blood pressure.
That’s why an annual physical with bloodwork to catch chronic disease early is so important, especially for anyone at high risk.
STOPPING IT EARLY
Understanding and managing your risk factors is the first step toward heading off kidney disease before the damage is done.
Anyone 65 and older living with diabetes, obesity, chronic high blood pressure, or heart disease should talk with their physician about their risk of developing kidney disease. So, too, should younger patients who are otherwise healthy but have a family history of kidney problems.
“Polycystic kidney disease is a fairly common hereditary disease where cysts form in the kidney and can replace much of the kidney,” Dr. Venkataraman says. “That, in turn, can lead to kidney failure.”
Treating kidney disease typically involves treating the underlying conditions that caused it, whether diabetes, high blood pressure, or an inherited condition.
Medications like ACE inhibitors for blood pressure and newer drugs like SGLT-2 inhibitors and semaglutide to manage diabetes are commonly prescribed to keep kidney disease in check.
“Beyond medications, there are other preventive steps we can take to protect our kidneys,” Dr. Venkataraman says. “Stopping smoking, limiting alcohol and salt intake, eating a healthy diet, and being physically active can help slow the progression of kidney disease.”