More than 25% of Americans suffer from gastroesophageal reflux disease (GERD), and some of those GERD patients — up to 10% of them — may contract a condition known as Barrett’s esophagus that greatly increases their risk of cancer.
“Patients who have Barrett’s esophagus are 30 times more likely to develop esophageal cancer than those who don’t,” says Abdul El Chafic, MD, gastroenterologist on the medical staff at Methodist Richardson Medical Center.
Barrett’s, a “pre-malignant” condition, is a complication of GERD in which the cells lining the lower esophagus become damaged by acid reflux. That’s a red flag for physicians like Dr. El Chafic, whose job involves treating the small fraction of Barrett’s patients who may develop cancer.
“The yearly incidence rate of cancer from Barrett’s is about 0.1% per year,” or 1 in 1,000 patients, Dr. El Chafic says.
But cases of esophageal cancer linked to Barrett’s have been on a steady rise in recent years, Dr. El Chafic says. But unlike colon or breast cancer, there’s no recommended standard screening for esophageal cancer. Most patients don’t even realize it’s cancer until a more alarming symptom emerges: the inability to swallow.
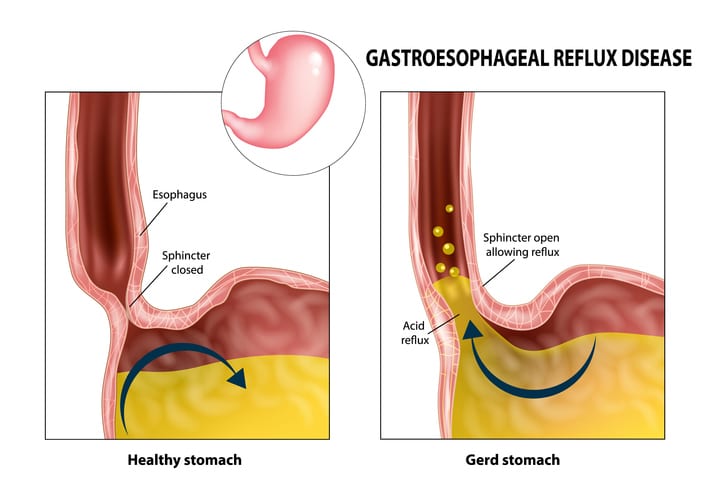
BARRETT’S ESOPHAGUS
Most people who experience acid reflux need not worry about Barrett’s, Dr. El Chafic says. It’s a condition that primarily affects a very small proportion of chronic sufferers.
“What happens is that stomach acid causes prolonged irritation in the lining of the esophagus and that results in a transformation of the cells there,” he says.
In other words, Barrett’s is generally the result of years of damage to the lower esophagus. The typical squamous cells of the esophageal lining transform into columnar cells, which are found in the stomach. The only way to confirm the diagnosis is to perform an endoscopic biopsy, which involves using a tube-like instrument to take a cell sample from the lower esophagus.
Patients who are diagnosed with Barrett’s need to have a follow-up endoscopy to make sure the cells do not become even more abnormal, or dysplastic.
“Dysplasia signals a precancerous stage,” Dr. El Chafic says.

RISK FACTORS
The only indication to examine a patient for Barrett’s is chronic acid reflux for more than 5 years, Dr. El Chafic says. Otherwise, it might be overlooked.
According to recently updated American College of Gastroenterology guidelines, men who are over 50, white, smokers, obese, and have a family history of Barrett’s or esophagus cancer are more likely to develop Barrett’s, Dr. El Chafic explains.
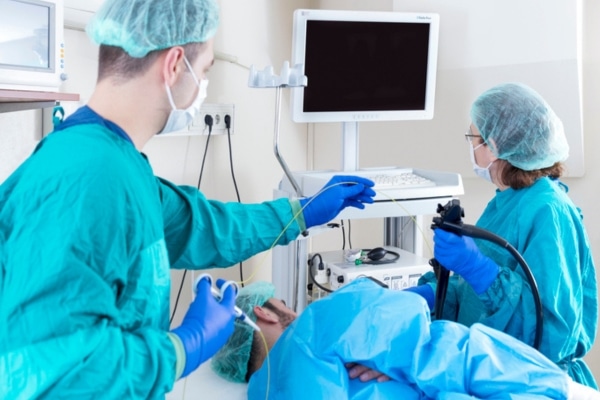
TREATMENT OPTIONS
The good news is that if doctors catch Barrett’s early enough, the progression can be halted before it worsens. The first line of defense is to make anti-reflux lifestyle changes — such as modifying your diet — and use proton pump inhibitors (PPI), or drugs that reduce acid production in the stomach. In certain circumstances, anti-reflux surgery may be recommended.
Still, if gastroenterologists do detect pre-cancer or cancer, they may be able to perform minimally invasive endoscopic procedures to remove the affected tissue, which can allow patients to avoid major surgery.
”Prevention is best,” Dr. El Chafic adds. “But in terms of treatment, we can do so much endoscopically now than ever before.”
While neither GERD nor Barrett’s is a guaranteed warning sign of cancer, some people may still benefit from a frank and open discussion with their physician.
“What is interesting for me as an advanced endoscopist is what we are capable of doing for the patient,” Dr. El Chafic says. “We have a lot of room to deal with a problem before it escalates, and that includes educating people and spreading awareness.”