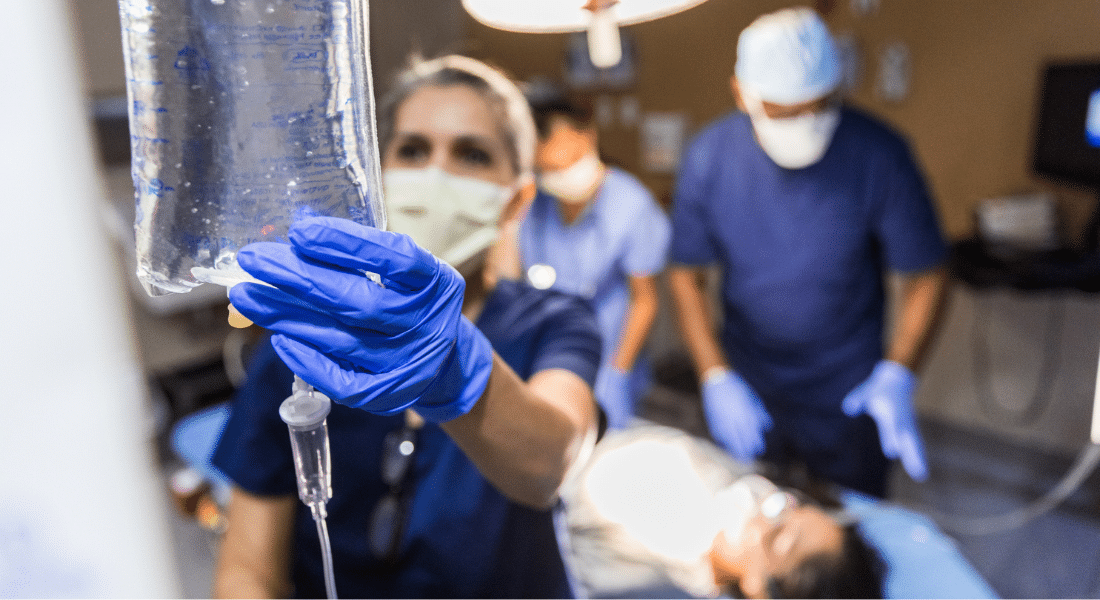
Sepsis claims more lives each year than diabetes and stroke combined, and yet few can name its symptoms, much less explain what causes it, according to a recent survey.
That’s why September has been designated Sepsis Awareness Month and why this year the Centers for Disease Control and Prevention launched a nationwide initiative to support the fight against sepsis at U.S. hospitals.
Methodist Health System is devoted to caring for patients with sepsis and has implemented an emergency department protocol and “Code Sepsis” alert to expedite care and combat sepsis mortality.
“We have activated a protocol when we suspect a patient may have sepsis,” says Brad Sellers, DO, vice chair of emergency medicine at Methodist Dallas Medical Center. “Code Sepsis alerts all of our doctors and nurses, but also the pharmacy, radiology, and the lab.
“There are a lot of departments that are involved in our septic care to make sure we are saving lives.”
MILLIONS DIAGNOSED
Often referred to as “blood poisoning,” sepsis is a life-threatening complication caused by an infection you already have. It occurs when chemicals released into the bloodstream to fight an infection trigger inflammation throughout the body.
The toll that sepsis takes each year is staggering: More than 1.7 million Americans are diagnosed with sepsis every year, nearly as many as are diagnosed with cancer. About 350,000 of those cases are fatal.
Sepsis affects patients of all ages, but older adults are especially vulnerable. Those 65 and older are 13 times as likely to be hospitalized with sepsis, compared with younger patients.
But young children, too, are among the hardest hit, with 20 million cases and 2.9 million global deaths among children under 5 years of age.
Other vulnerable patient populations include:
- Pregnant women
- People with chronic conditions like diabetes, kidney or lung disease, and cancer
- Patients with a weakened immune system or who recently used antibiotics or steroids
- People with wounds or other injuries
WHAT ARE THE SYMPTOMS?
Since sepsis can affect different areas of the body, there are many possible symptoms. They include:
- Fast heart rate
- Low blood pressure
- Fever or hypothermia
- Shaking or chills
- Warm or clammy/sweaty skin
- Confusion or disorientation
- Shortness of breath
- Cellulitis or rash
- Extreme pain or discomfort
Other common symptoms include urinary issues such as the urge to urinate or reduced urination.
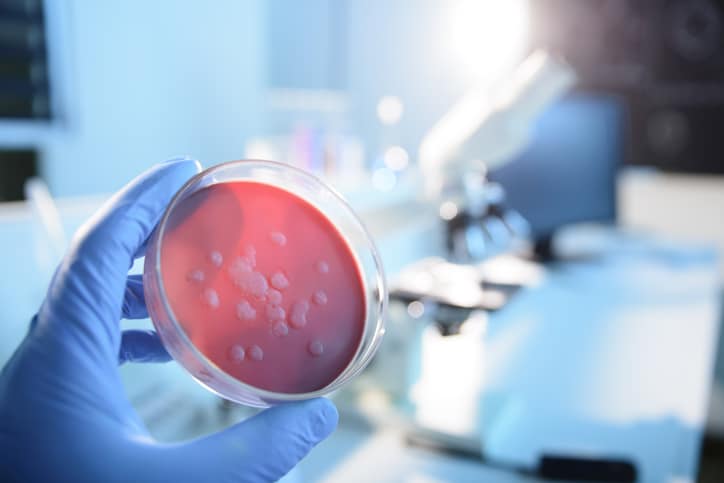
RESISTANT TO ANTIBIOTICS
Sepsis can affect anyone, but people with an infection — such as bacteremia, or bacteria in the blood — are especially susceptible. That often means a staph infection, and when that infection is resistant to antibiotics, it’s referred to as MRSA, or methicillin-resistant Staphylococcus aureus.
“Sepsis, most of the time, starts in the community because MRSA is already in the community,” Dr. Sellers says. “There’s a large number of people that are carriers of MRSA that already have it, and they don’t even know it because we don’t test everybody.”
Healthcare providers identify sepsis on a scale that ranges from infection and bacteremia to sepsis and septic shock, which can lead to the dysfunction of multiple organs. In severe cases, sepsis causes a dangerous drop in blood pressure, which doctors call “septic shock.”
Septic shock can quickly lead to organ failure, such as your lungs, kidneys, and liver.
“If you have sepsis, you want to come in immediately before it becomes septic shock. It’s really important to come in early and let us check you if you think you may have a fever, low body temperature, a fast heart rate, a urine infection, or cellulitis,” Dr. Sellers says.

HOW TO STOP SEPSIS
Raising awareness and preventing infection, to begin with, are critical to the fight against sepsis.
That could mean practicing good hand hygiene and keeping cuts and other wounds cleaned and covered. Staying up to date on recommended vaccines is also important because sepsis can begin with any infection.
Once a patient is diagnosed, treatment should begin immediately because sepsis spreads quickly in the bloodstream. A patient may receive antibiotics, IV fluids, and other medications, or they may require surgery to remove tissue damaged by the infection.
“With quick diagnosis and treatment, many people with mild sepsis survive,” Dr. Sellers says.