Pregnancy causes drastic changes in a woman’s hormones, including insulin, and for some patients that can result in gestational diabetes.
Insulin is the hormone made by the pancreas that acts as a key to letting blood sugar or glucose move from the blood and into the cells to produce energy.
The condition usually develops around the 24th week of pregnancy and goes away after the baby is delivered. If it doesn’t go away after birth, then it’s called type II diabetes.
Gestational diabetes can be dangerous for the baby and mother, especially when left untreated. It raises the risk of stillbirth and can be associated with high blood pressure during pregnancy, also known as preeclampsia.
It can also cause a baby to grow so large in the womb that the mother has a higher risk of needing a cesarean section. The problems may not stop at delivery for the child, who may experience breathing issues or jaundice immediately after birth, and diabetes later in life.
It’s not all bad news, however, especially with an OB-GYN like Dr. Johnson to help guide the way.
“If you’re diagnosed with gestational diabetes,” she says, “just know there are plenty of ways to manage it.”
WHO’S AT RISK?
As you might suspect, women are predisposed to this condition if they are pre-diabetic or suffered from gestational diabetes during a previous pregnancy.
Women are also at higher risk if their body mass index is above 25, classified as overweight, or obese, a BMI of 30 or more.
You may also be at higher risk for gestational diabetes if you:
- Are physically inactive
- Had gestational diabetes in a previous pregnancy
- Had a large baby in a past pregnancy
- Have high blood pressure
- Suffer from heart disease
- Have polycystic ovary syndrome
- Have an immediate family member with diabetes
- Are Black, Native American or Alaska Native, Asian, Hispanic/Latino, or Pacific Islander
What’s more, you may not have any of these risk factors and still develop gestational diabetes.
“That’s why we regularly test pregnant women for it,” Dr. Johnson says.
The good news is there are ways to help prevent gestational diabetes. Here are five tips to keep it in check:

1. GET TO A HEALTHY WEIGHT
If you’re planning to get pregnant soon, Dr. Johnson recommends you aim to maintain a BMI of 25 at most. A key risk factor is starting your pregnancy overweight or obese.
“If your BMI is between 25 and 29.9, we recommend you gain a maximum of 25 pounds during pregnancy,” Dr. Johnson says. “If your BMI is over 30, the maximum we want you to gain is 20 pounds.”
If your BMI is healthy (under 25) at the outset, she adds, gaining up to 35 pounds should be OK.
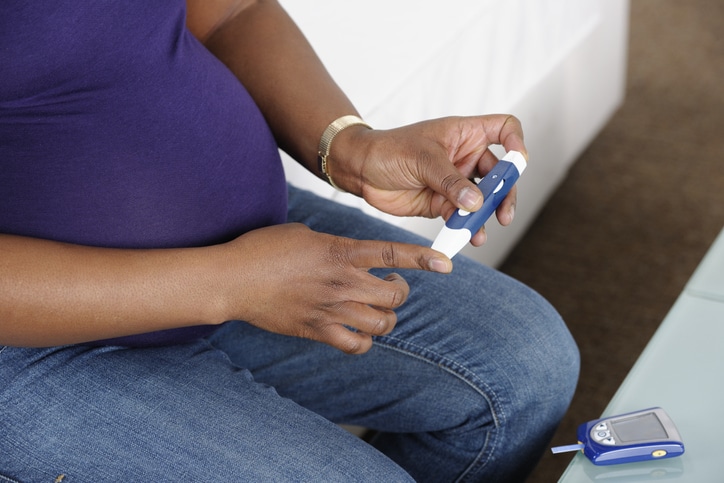
2. TEST YOUR BLOOD SUGAR
Healthy blood sugar levels differ depending on the last time you ate a meal, but in general, it ranges from 80 to 140 milligrams per deciliter before a meal and under 140 two hours after a meal.
If you are diagnosed with gestational diabetes, staying under 140 mg/dL will be easier if your OB-GYN tests your blood sugar levels early and regularly.
“If you are diagnosed with gestational diabetes, your doctor will prescribe an at-home glucose monitor to help you keep a close eye on your blood sugar,” Dr. Johnson says.
She advises her patients to check their blood sugar at least four times a day, especially after meals, to make sure their levels stay within a healthy zone. This will help prevent the adverse effects that could develop with gestational diabetes.

3. SAY NO TO PROCESSED FOODS
A diet that focuses on fresh whole foods instead of processed foods can help you keep your blood sugar in check.
“The processed foods you should avoid include sweets, packaged foods, processed meats, microwave-ready meals, cereals, and granola bars if their added sugar content is high,” Dr. Johnson says.
The problem with highly processed foods is, they are usually loaded with sodium to prolong their shelf life, as well as sugar and added fats to make them taste better.

4. WORK OUT
If you had a fitness routine before getting pregnant, DON’T STOP! If you didn’t, then now is a good time to start.
Try taking 30-minute walks three times a week, for starters. Or find a low-impact exercise you enjoy like swimming or a Zumba dance class. The key is boosting your heart rate and burning off calories, while still keeping you and your baby safe.
“If you’re pregnant avoid contact sports,” Dr. Johnson says. “You can easily get hit in the stomach while playing these sports and could harm your baby.”

5. EAT MORE FIBER
High-fiber foods such as whole grains, beans, lentils, broccoli, and apples can help manage blood sugar and maintain a healthy weight. So naturally, they can help you dodge gestational diabetes, too.
“Women who eat a low-fiber diet have twice the chance of developing gestational diabetes,” Dr. Johnson warns. “So do your best to eat a high-fiber diet.”
Finally, when dietary changes and other precautions don’t do the job alone, there are prescription drugs to help maintain healthy blood sugar levels.
“If healthy lifestyle changes aren’t enough to manage your blood sugar,” Dr. Johnson says, “your doctor may prescribe insulin, metformin, or other medications to help manage your blood sugar.”






