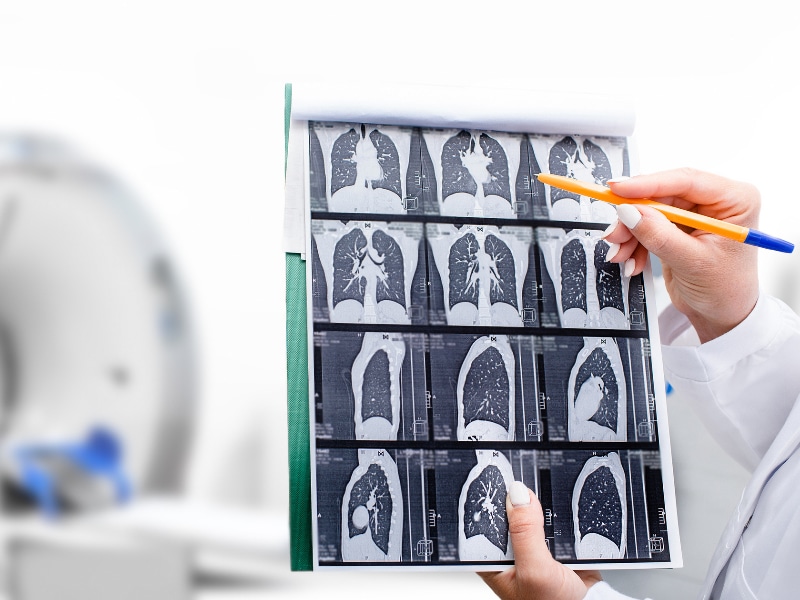
Lung cancer claims more American lives each year than colon, breast, and prostate cancers combined, and with thousands of new cases reported each year, annual screenings are a must for patients who are most at risk.
Diagnosing the disease at the earliest stage possible is critical to effective treatment, says David Mason, MD, thoracic surgeon on the medical staff at Methodist Dallas Medical Center.
“One of the reasons lung cancer is so deadly is because it’s often found in an advanced stage,” Dr. Mason says. “The lungs have no pain receptors, so something can sit there silently for quite some time. In most cases, you only notice symptoms when it has spread.”
The good news is we have proven tools at our disposal to catch any potentially cancerous masses — starting with a simple, noninvasive CT scan — and treatments are plentiful and constantly advancing.
“For people treating lung cancer like myself, there’s never been more optimism than there is right now,” Dr. Mason says. “The last decade has really been a revolutionary period for advancements in lung cancer.”
Dr. Mason answered some of the most frequently asked questions about risk factors and screening guidelines.
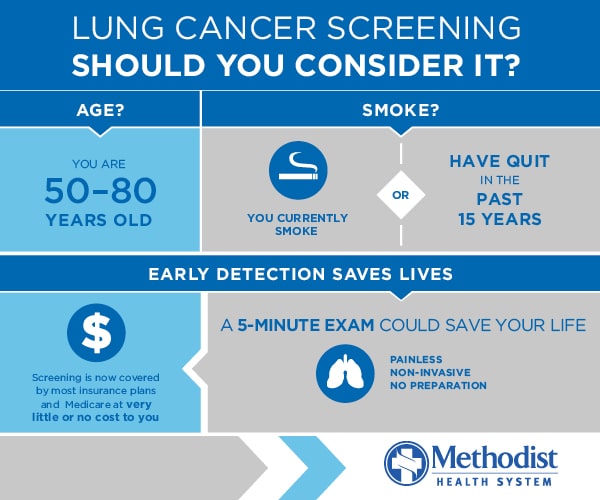
WHO SHOULD GET SCREENED?
Of course, we can’t talk about lung cancer without also mentioning its link to tobacco use. Tobacco products contain a staggering list of chemical compounds — many of which are known carcinogens, including lead, formaldehyde, and arsenic, an ingredient famously used as rat poison in the 20th century.
So it’s no wonder that smoking, which accounts for 80% to 90% of lung cancer cases in the U.S., remains the top risk factor today, according to the Centers for Disease Control and Prevention.
“That’s why we recommend screening for people who are 50 to 80 years old, currently smoking or have quit in the last 15 years, and have a smoking history that spans, on average, one pack a day for 20 years,” Dr. Mason says.
This is because the risk is largely based on cumulative years of smoking, according to the Journal of the American Medical Association. For these high-risk individuals, getting screened can be potentially life-saving.
But because of the stigma associated with smoking, it can make it hard for physicians to catch lung cancer early.
“So often, lung cancer gets stigmatized as a self-inflicted malignancy. That can prevent people from getting the care they need,” Dr. Mason says. “That’s a big problem.”

WHAT ABOUT NON-SMOKERS?
Tobacco use undoubtedly puts you in greater danger, but it would be wrong to assume lung cancer is only a smoker’s disease. In the U.S., 10% to 20% of lung cancers are found in people who rarely or never smoked, according to the CDC.
Studies show other environmental factors, such as exposure to certain chemicals like radon and asbestos, and family history can cause lung cancer, among other diseases.
Researchers also dispute the misconception that lung cancer is a disease of older adults. In a study of 173,856 patients, 5,657 of them were 20 to 46 years old.
But non-smokers and young people make up a small group of patients, Dr. Mason says, so the pros and cons of screening should be weighed on a case-by-case basis.
Because there is a concern of overdiagnosis and repeated exposure to X-ray radiation — even in such small amounts — the screening process for lung cancer primarily aims to help people who face the greatest risk of disease.
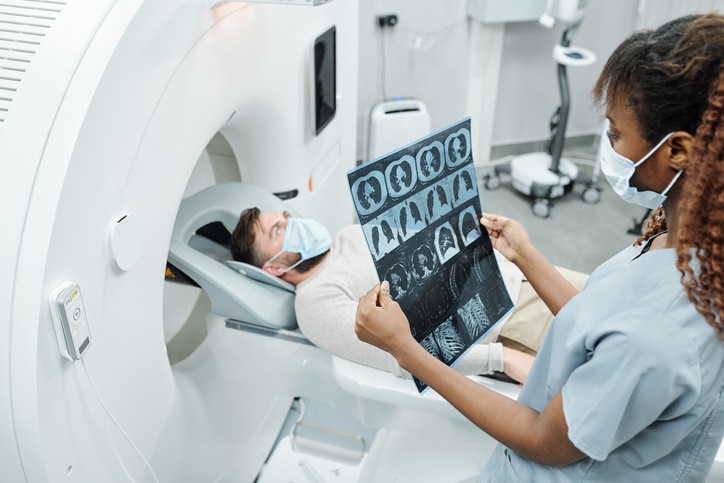
WHAT DOES A LUNG CANCER SCREENING INVOLVE?
It can all seem overwhelming and stressful, but at hospitals like Methodist Dallas offer the services of patient navigators like Joli Uetrecht, MSN, RN, who help guide people through screening, diagnosis, treatment, and follow-ups.
If you’re the type of person who gets squeamish about doctor visits, you can rest assured that the screening process is as simple as it gets.
“We use a low-dose CT scan,” Dr. Mason says. “You lie down, and the X-ray takes only a few minutes to complete.”
This noninvasive procedure uses a very low dosage of radiation to produce scans of the lungs.
“It’s the most established method of screening for lung cancer,” Dr. Mason explains.

How is lung cancer treated?
Nowadays, depending on the stage and type of cancer, patients can benefit from multiple treatment options that range from traditional to innovative.
“Surgery, radiation, and chemotherapy still play a big role,” Dr. Mason says. “We also have new targeted therapies and immunotherapy that attack specific cancer cells.”
And many of the medications can be taken by mouth at home, as opposed to the clinical infusions that require more planning and commitment. This makes it easier on patients, especially as many of the medications have milder side effects, Dr. Mason adds.
“And many of these therapies will probably be applicable to people who have even earlier stage cancers,” he says. “There’s still a lot to learn, but the good news is we have real and effective treatments for everybody now.”