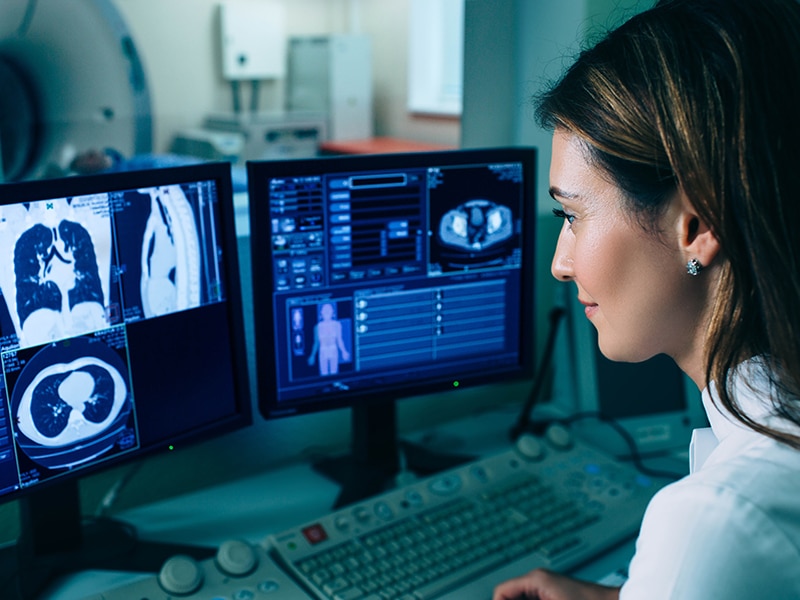
For the vast majority of people who come down with COVID-19, a diagnosis means a couple of weeks of coughing, fever, and difficulty breathing.
“About 80% of the cases are considered mild and patients able to fully recover at home,” says Ed Dominguez, MD, an infectious disease physician on the medical staff at Methodist Dallas Medical Center.
But does everyone really fully recover? It’s still early in this pandemic, but doctors are seeing evidence that there may be some lasting health effects due to this virus.
Lungs
COVID-19 patients who develop acute respiratory distress syndrome and have to be in the intensive care unit are more likely to have long-term consequences.
“If symptoms are serious enough, doctors have to rely on ventilators to provide life support and help patients breathe,” says Zachary Dreyfuss, MD, MPH, a pulmonologist and critical care physician on the medical staff at Methodist Dallas.
“Heavy sedatives and pain medications are needed for patients to even tolerate being on a ventilator because it’s extremely uncomfortable,” Dr. Dreyfuss says.
What’s more, he says, patients who need help breathing won’t be using the muscles we all use every day without even thinking about it.
“This leads to weakness,” Dr. Dreyfuss says. “Many patients who leave the intensive care unit (ICU) are extremely debilitated and face a long course of recovery.”
Heart
Dr. Dominguez says recent reports from China indicate a higher rate of heart problems in COVID-19 patients who have recovered.
In fact, roughly 20% of coronavirus patients in China had heart damage during hospitalization, a recent study found.
Another study discovered about 16% of patients developed an arrhythmia, while other reports indicated cases of acute onset heart failure, heart attack, and cardiac arrest after infection, the American College of Cardiology states.
Kidneys
There’s no evidence COVID-19 hurts the kidneys of people who have mild to moderate infection, but kidney abnormalities have been seen in 25–50% of patients who develop the severe type of the disease, according to the International Society of Nephrology.
Those patients have more protein and red blood cells in their urine. About 15% of them also develop a decline in kidney filtration function.
“COVID-19 can put a great deal of strain on the kidneys, even requiring dialysis in extreme cases,” Dr. Dreyfuss says.
Brain
It may be too early to know exactly what patients will face years down the road. But we do know how challenging a stay in intensive care can be.
Life in the ICU — with its potent medications, frequent checkups, and the concert of disconcerting noises — can also interfere with patients’ sleep and leave them feeling emotionally strained and disoriented.
“When some people leave the ICU, there are lasting effects similar to a post-traumatic stress disorder,” Dr. Dreyfuss says.
Follow-ups matter
Whether it’s dealing with the mental health stress of recovery or following up on lingering symptoms, tackling a treatment plan isn’t a one-size-fits-all situation. That’s why Dr. Dominguez encourages patients recovering from COVID-19 to consult a trusted source, starting with their primary care providers.
“It is important, regardless of how sick you were with COVID-19, to speak with your doctor and determine how frequent any follow-up should be based on your underlying health prior to infection,” Dr. Dominguez says.
4 unusual symptoms of COVID-19