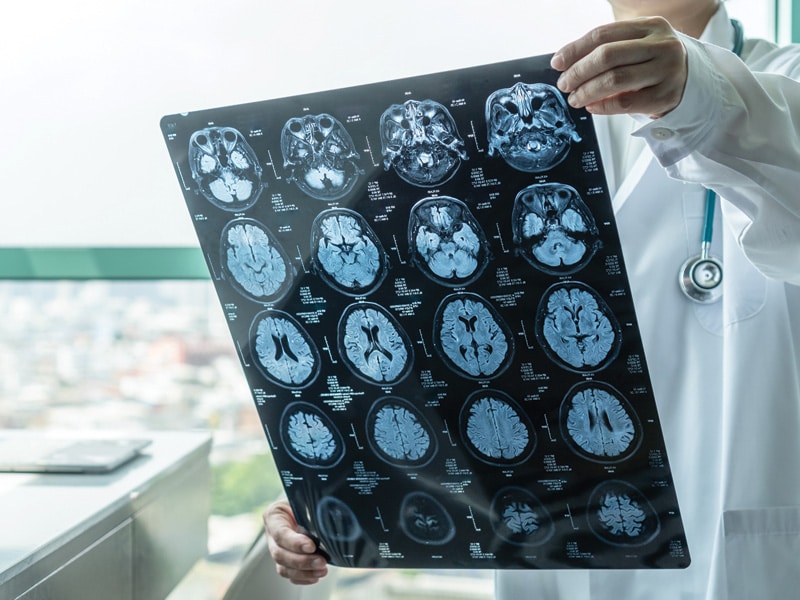
The coronavirus isn’t picky about which organs it attacks, from the heart and lungs to the kidneys, digestive system, and even the brain.
The threat of strokes makes the brain especially vulnerable to COVID-19.
A stroke can occur when a blood clot cuts off the flow of oxygen to the brain. And COVID-19 excels at creating blood clots.
“The coronavirus causes generalized inflammation in blood vessels throughout the body. This condition makes it easier for clots to form,” explains Bartley Mitchell, MD, neurosurgeon on the medical staff at Methodist Dallas Medical Center.
Most people hospitalized for stroke are 65 or older, according to the Centers for Disease Control and Prevention. But doctors are reporting an increase in stroke cases in younger people with COVID-19.
“We’re seeing patients with COVID-19 who are younger than 50, who have no risk factors, presenting with strokes,” Dr. Mitchell says.
MEDICAL EMERGENCY
Depending on which part of the brain is affected, strokes can cause severe damage, such as muscle paralysis, vision problems, speech issues, and memory loss.
“It’s critical to get to a hospital if you think you or someone else is having a stroke,” Dr. Mitchell says.
In short, BE FAST about seeking medical help when these stroke symptoms arise:

Calling 911 is critical because EMTs and paramedics are trained to recognize stroke victims and provide helpful interventions, Dr. Mitchell says. They also know which hospital has the level of stroke care the patient needs.
“The top level is a comprehensive stroke center, which is what we have here at Methodist Dallas,” he says. “This means that we can provide all of the major treatments that are available for stroke patients.”
If patients get to the hospital within 4 1/2 hours of their stroke, doctors can administer medications to break apart the clot. They can also give anticoagulants or blood thinners to stop others from forming.
Beyond that window, physicians have other avenues of resolving the blockage.
“That’s really where the advancements in technology have taken place over the past five years,” Dr. Mitchell says. “We can do more and be effective in turning people’s symptoms of a stroke around.”
But the sooner you get help the better because turning the damage around is another matter.

SAFETY IS A PRIORITY
A chilling result of the pandemic is the sharp decline in emergency department visits. Doctors are concerned people are avoiding urgent medical care out of fear of being exposed to COVID-19.
“Many people with stroke symptoms are not coming to the hospital. And that’s a problem because, by the time they do come to the hospital, we can’t do anything about it,” Dr. Mitchell says.
Dr. Mitchell says delaying care is an unnecessary gamble because hospitals have taken every precaution to prevent the spread of COVID-19 among both staff and patients.
At Methodist, everyone who comes through the door is screened for COVID-19 symptoms before admission, and infected patients receive help in a separate unit cordoned off from the rest of the hospital. What’s more, a special ventilation system keeps any potential viral particles from circulating to other areas.
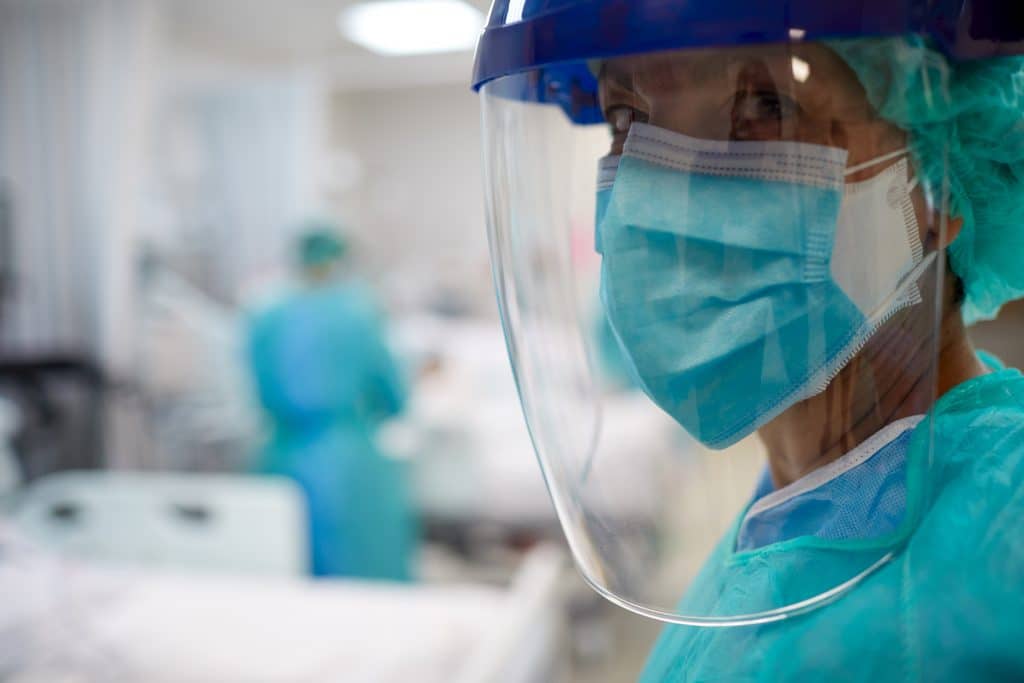
“The staff caring for our COVID-19 patients wear a full gamut of personal protective equipment — meaning masks, eye shields, gloves — and follow a strict handwashing and sanitization protocol throughout these areas,” Dr. Mitchell says.
REDUCING RISK
If you’ve been exposed to COVID-19 and want to reduce your risk of stroke, the best recommendations may sound familiar: maintain a healthy blood pressure, lower your cholesterol, refrain from smoking, and exercise regularly.
And because people with diabetes are also at a heightened risk, it’s important for those patients to monitor their blood sugar and insulin levels.
“The primary things that can help people to prevent strokes are things that we have control over,” says Dr. Mitchell, who advocates for healthy lifestyle changes and physician-approved medications to help manage risk factors.
Meanwhile, health experts emphasize the importance of getting vaccinated and continuing to practice those familiar precautions — covering your face, washing your hands, and socially distancing — whether you’re vaccinated or not.
“What we have learned about treating COVID-19 is just phenomenal,” Dr. Mitchell says. “But these protective measures are still important, and I encourage all of my patients, friends, and family to stick with them.”
COVID-19 afflicts the young, too, causing blood clots and even strokes.