When health officials first approved Paxlovid to treat COVID-19, it was touted as the most effective way of heading off severe infection and hospitalization. Now preliminary research shows that it could also prevent long COVID-19.
Patients who took the anti-viral were less likely to suffer persisting symptoms like fatigue, cardiovascular problems and brain fog, according to a large study that used data from a Veterans Health Administration database.
The drug limits how the virus replicates when it’s taken within five days of experiencing COVID-19 symptoms.
“Paxlovid reduces the number of copies of the COVID virus, thus reducing deep-tissue penetration and prolonged disease,” says Jon Albrecht, RPh, MHA, BCNSP, FASHP, vice president of Pharmacy Services for Methodist Health System. “That’s why it is important to take it early when symptoms first appear.”
In this way, the pill works much like Tamiflu, another anti-viral medication, does for the flu, which must also be taken within the first five days of symptom onset.
“What we’re trying to do is prevent the virus from replicating, whether you’re talking about Tamiflu with the flu virus, or whether you’re talking about COVID-19,” Albrecht says. “If you have too much virus in your body, it’s not going to be as effective.”
Albrecht and other experts break down the data on this “game-changer” that’s become the go-to treatment for high-risk patients:
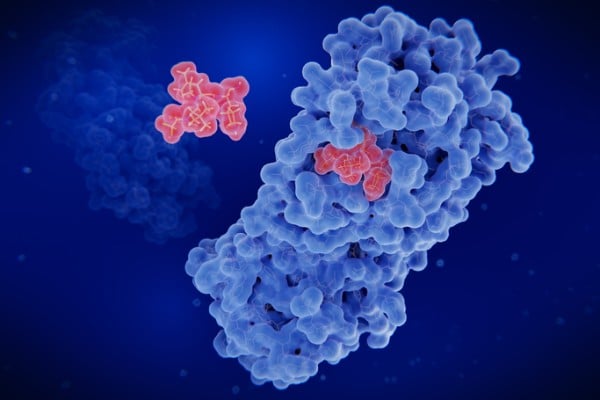
HOW DOES IT WORK?
Even if you’re familiar with Paxlovid, you may not know that it consists of two distinct drugs with two distinct purposes:
- Nirmatrelvir stops the infection in its tracks by inhibiting an enzyme that the coronavirus needs to replicate.
- Ritonavir, a drug that has been used to treat HIV/AIDS, prevents the liver from metabolizing nirmatrelvir so it stays in the body longer.
But most people know the drug for its peculiar aftertaste known as “Paxlovid mouth” and for the fact that some patients experience a “COVID rebound” after they stop taking the medication.
When President Joe Biden and his chief COVID-19 advisor, Anthony Fauci, took Paxlovid last winter, they both had a quick recovery. But they also suffered rebound infections days afterward. Biden reported a mild cough the second time, while Fauci said his second bout was worse than the first.
It’s likely that the infection re-emerges in older patients because the virus burrowed into tissues, where the anti-viral could not easily penetrate, says Jon Albrecht, RPh, MHA, BCNSP, FASHP, vice president of Pharmacy Services for Methodist Health System.
“The coronavirus can be deep-seated within tissues,” Albrecht says. “So if you stop taking the drug before the virus is fully suppressed, then it starts to replicate again.”
Albrecht adds that Paxlovid’s components, nirmatrelvir and ritonavir, may cause other symptoms such as abdominal pain, nausea, and malaise, which are common with most anti-viral drugs.
The Centers for Disease Control and Prevention issued a health alert in May 2022, saying rebound symptoms were typically mild and no cases were severe.

WHO CAN GET PAXLOVID?
First approved for emergency use in December, Paxlovid was in high demand during the winter surge. Now, it’s widely available, with a doctor’s prescription, and pharmacists are more worried that thousands of doses will go to waste.
That’s because the U.S. government bought 20 million courses of Paxlovid in April 2022 to be distributed at selected pharmacies.
“Paxlovid is available from both the Methodist Dallas and Charlton Community Pharmacies, which will deliver to a patient’s home free-of-charge,” Albrecht says of the 30-capsule, five-day oral medication.
You don’t have to be the most powerful man in the free world to get a prescription for Paxlovid, but this anti-viral medication is not for just anyone either.
Paxlovid is authorized for people 65 and older or people 12 and up with mild to moderate COVID-19 who may be at high risk of severe disease, according to the FDA.
“The best results have been seen in patients 65 and older,” Albrecht says.

HOW EFFECTIVE IS IT?
Paxlovid isn’t the only anti-viral approved for treating patients at high risk for COVID-19. But it’s proved to be the most effective – by far.
Remdesivir, the only COVID-19 anti-viral treatment that has gained the full approval of the FDA, has been part of our COVID-19 arsenal since early in the pandemic. But it must be administered by IV for three consecutive days, so its use has been reserved for hospitals, assisted-living facilities, and home healthcare.
“We probably would use it more if it was easier to administer,” Albrecht says.
Molnupiravir is an oral medication that hit the market a month ahead of Paxlovid. Like its competitor, it prevents the virus from multiplying and must be taken for five days, within five days of symptom onset.
But both anti-virals are not equal: Molnupiravir is about 30% effective at preventing hospitalizations, data indicate, whereas Paxlovid reduced the risk by nearly 90%. That lower efficacy has made doctors reluctant to prescribe molnupiravir unless Paxlovid is unavailable.
DRUG INTERACTIONS
One downside of Paxlovid is the laundry list of other medications it can interact with, many of them drugs that older adults depend on.
That’s because the same ingredient that pumps up the anti-viral component of Paxlovid also gives a potentially unsafe boost to drugs that treat heart arrhythmia, cancer, and epilepsy, among others.
Drugs that treat cancer, high cholesterol, and an enlarged prostate are also on the list, as are blood thinners, which can reach unsafe levels in the body because the drug interferes with their metabolism. President Biden reportedly switched to low-dose aspirin and stopped taking a blood thinner and cholesterol drug during his treatment.
It’s wise to share a list of your medications with a doctor or pharmacist before seeking a prescription for the anti-viral.

VACCINATE, THEN TEST
Treating a potentially serious infection is no substitute for preventing it, so being up to date on your COVID-19 vaccinations (including those all-important boosters) is just as important as ever.
The vaccines may not prevent you from getting sick, especially with the highly contagious BA.5 variant going around, but they should protect you from the worst effects of COVID-19, potentially including “long COVID.”
And remember, medications like Paxlovid have a very short window of effectiveness, so if you’re at high risk and you feel sick, get tested as soon as possible. Don’t shrug off your symptoms as allergies or a run-of-the-mill cold.
“Better safe than sorry,” Albrecht says. “Go get tested and check in with your doctor. They will know what to do.”

