Hernias are among the most common surgical conditions, with more than 1.5 million diagnosed each year. They can affect anyone, from newborns to the very old, and can be life-threatening if left untreated.
Men are up to 10 times more likely than women to get a hernia, which is what happens when an internal organ or tissue like fat protrudes through a weak spot in the abdominal muscles.
Many people may have been at risk of a hernia since birth, and their lifestyle choices raise that risk, says Joe Radzevich, DO, general and bariatric surgeon on the medical staff at Methodist Southlake Medical Center.
“Most groin hernias are caused by the incomplete closure of the inguinal canal during development,” Dr. Radzevich says. “The risk increases with things like strenuous activity, heavy lifting, chronic coughing due to smoking, straining due to chronic constipation, and obesity.”
Dr. Radzevich discussed hernias and the benefits of robotic surgery during a presentation to Methodist Generations, an education and enrichment program for older adults.
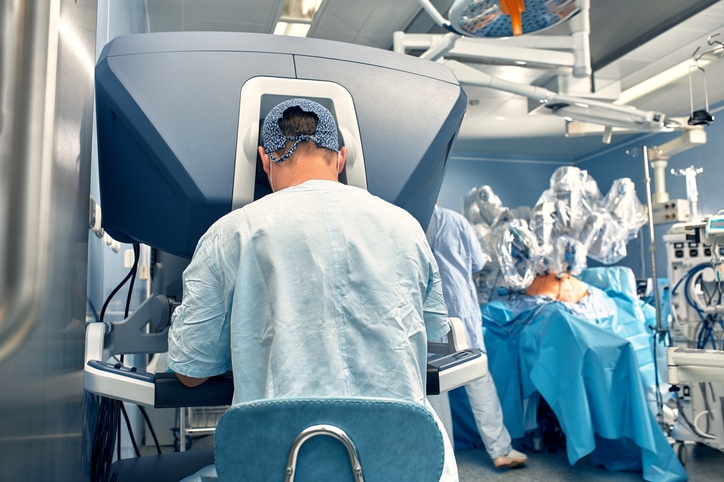
A surgical robot puts advanced imaging and high-precision tools at a surgeon’s fingertips.
WHEN TO SEEK HELP
Surgery is the only way to fix a hernia. While it may not require urgent repair, a hernia can become an emergency when the organ or tissue gets trapped outside the abdomen, and its blood flow gets cut off.
“With an incarcerated or strangulated hernia, there’s a danger of obstruction and even tissue death if the blood supply is cut off,” Dr. Radzevich says. “That’s when you should seek immediate medical attention.”
Ignoring a hernia can have serious consequences. Signs of a strangulated hernia include:
- Nausea
- Fever
- Redness and tenderness at the hernia site
- Severe, persistent pain
- Vomiting
Trust your gut to advanced GI care at Methodist by finding a digestive health specialist near you. Visit MethodistHealthSystem.org
TYPES OF HERNIAS
Inguinal: Accounting for 75% of all hernias, inguinal hernias are often congenital, caused by the incomplete closure of the inguinal canal in the groin. Surgery might not be necessary immediately.
“For men who have no symptoms or are minimally symptomatic, watchful waiting is appropriate,” Dr. Radzevich says. “After three years, about 40% will need surgery.
Ventral: Another common type of hernia, these occur when the intestines protrude through the upper abdomen and include umbilical (near the belly button), epigastric (above the belly button), and incisional hernias, a side effect of a previous surgery.
“These hernias are often the result of strenuous activity or obesity,” Dr. Radzevich says. “We like for obese patients [BMI of over 40] to lose weight before surgery to lower the risk of another hernia.”
Femoral: A less common type, these hernias are more common in women and occur when fatty tissue pokes through into the femoral canal, below the inguinal canal.
Hiatal: These hernias, usually the result of acid reflux, occur when the top of the stomach bulges through the opening where the esophagus passes through the diaphragm.
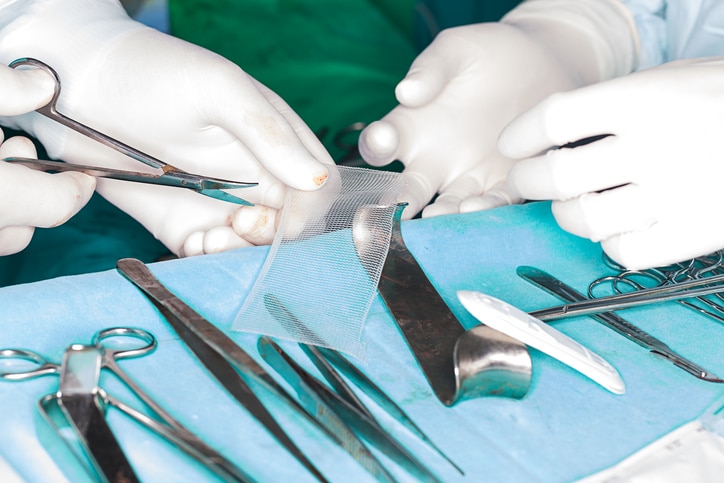
Surgeons use mesh to seal off the abdominal wall after repairing a hernia.
SURGICAL METHODS
There are three methods to repair a hernia surgically:
- The traditional open approach with an incision at the site of the hernia
- Laparoscopic using smaller incisions, a scope, and a camera
- Robotic-assisted, where the surgeon controls robotic surgical instruments while sitting at a console with a 3D display.
“The robotic platform lets surgeons see things a lot better,” says Dr. Radzevich, who performs almost all of his hernia surgeries with the da Vinci Surgical System. “The instruments move in ways that the human hand and arm cannot.”
Laparoscopic surgery has its place, but it’s limited because the tools are essentially “straight sticks” that can’t match the articulation of a robot.
“It’s certainly an approved method that has good results,” Dr. Radzevich says, “but I believe that the robotic approach is slightly better.”
Robotic hernia repair is often performed on an outpatient basis, with the patient in and out of the hospital the same day. Recovery times often prove shorter, as well.
“Smaller incisions leads to a faster recovery time and less pain,” Dr. Radzevich says. “It means you can get back to your normal life faster.”
Surgery may not be the best option immediately, and talking to a physician to learn about all the alternatives is always the first step.
“I like to approach each patient as an individual,” Dr. Radzevich says. “I don’t believe in a cookie-cutter, one-size-fits-all approach.”






