High blood pressure is known as a “silent killer” because it can go unnoticed for years while damaging blood vessels and vital organs — and that includes the brain, as well as the heart.
“What’s good for the heart is good for the brain,” says Akash Ghai, MD, cardiologist on the medical staff at Methodist Charlton Medical Center. “There’s emerging evidence that untreated hypertension in your 40s and 50s increases the risk of cognitive decline in your 70s.”
New guidelines released in 2025 by the American Heart Association place a renewed emphasis on that heart-mind connection, as well as early intervention by establishing a lower level for Stage 1 hypertension (130/80 mmHg).
Studies show that about one in five adults with hypertension are unaware they have the condition. In addition to causing cognitive issues, unchecked high blood pressure can cause heart attacks, strokes, kidney disease, and vision problems, says Nasser Khan, MD, FACC, FSCAI, medical director of the Structural Heart Program at Methodist Dallas Medical Center.
“Hypertension is called the silent killer because your arteries are being damaged silently while you’re undiagnosed,” Dr. Khan says.
Dr. Ghai and Dr. Khan explain the new guidelines, the best ways to put a lid on blood pressure, and how to take your heart (and brain) health into your own hands.
HOW GUIDELINES CHANGED
Blood pressure is the force with which blood flows through blood vessels to the heart and other parts of the body.
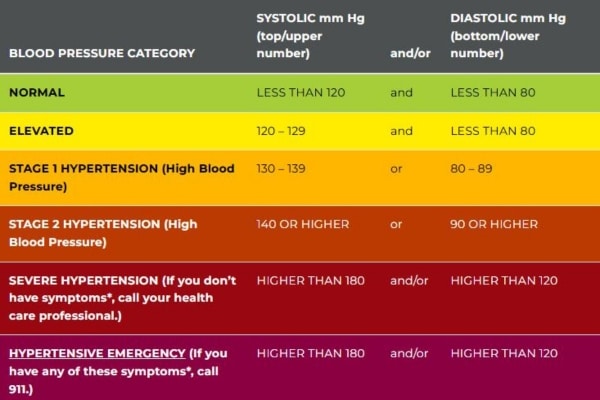
A normal blood pressure reading is below 120 for systolic (the upper number) and below 80 for diastolic (the lower number). If one or both numbers are higher than normal, it means your heart is having to work harder than it should to pump blood through your body.
Beyond setting a lower “universal target” of 120/80 mmHg, the latest guidelines shorten the window for controlling blood pressure with lifestyle changes alone to three to six months, encouraging doctors to turn to medical therapy sooner.
“If diet and exercise are not effective in lowering blood pressure, we should start at least one medication, according to those new guidelines” Dr. Ghai says.
Dr. Ghai also noted the new focus on cognitive decline as an eventual effect of years of untreated hypertension. That risk is proving to be an effective motivator for some patients.
“The guidelines are trying to help motivate people to get their blood pressure under control,” Dr. Ghai says. “There are some patients who are less worried about a heart attack but are more worried about getting dementia and losing their memory.”
When is the last time you took a beat? Watch our women’s Heart Month webinar. Visit MethodistHealthSystem.org
LOWERING BLOOD PRESSURE
About those lifestyle changes, both doctors offered some advice on the best ways to get high blood pressure under control by staying active and keeping a close eye on what we eat.
“Eat a heart-healthy diet with more fruits and vegetables, and cut salt to 1 to 2 grams of salt — no more than a teaspoon full,” Dr. Khan says. “Combine that with about 150 minutes a week of moderate-intensity exercise.”
Alcohol also plays a major role in hypertension, says Dr. Ghai, who doesn’t put much stock in the outdated notion that moderate drinking can protect your heart.
“New research pours cold water over that idea,” he says. “Alcohol can drive blood pressure up by constricting arteries, increasing weight gain, and worsening sleep apnea. So I recommend that patients abstain from alcohol.”
The first step to controlling hypertension is understanding your blood pressure. Knowing those numbers — and addressing high blood pressure early — is one of the most powerful steps we can take to protect your health.

KEEPING TABS AT HOME
Doctors have long understood the limitations of checking blood pressure at a single point in time, especially if that moment is at a clinic when a patient is already under the weather or anxious about visiting the doctor.
“It’s a good idea to buy a blood pressure cuff at home to check your own blood pressure,” Dr. Khan says.
That’s partly because some patients experience a phenomenon known as “white coat hypertension,” where their blood pressure readings in the clinic are elevated because of anxiety. On the flip side, “masked hypertension” occurs when blood pressure appears normal in the clinic but is elevated at home.
Dr. Khan recommends an upper-arm cuff that’s been validated for accuracy by the American Medical Association.
“Home blood pressure monitoring is increasingly recommended as an important tool to confirm diagnoses,” he says.